Excess iodine exposure acutely increases salivary iodide and antimicrobial hypoiodous acid concentrations in humans - Scientific Reports
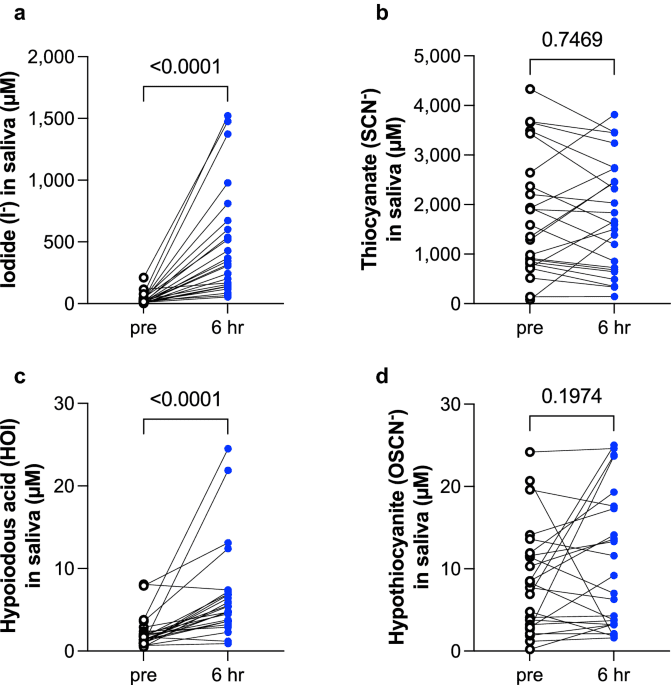
The lactoperoxidase (LPO)-hydrogen peroxide-halides reaction (LPO system) converts iodide and thiocyanate (SCN−) into hypoiodous acid (HOI) and hypothiocyanite (OSCN−), respectively. Since this system has been implicated in defense of the airways and oropharynx from microbial invasion, in this...
This study shows that taking iodine increases the formation of hypoiodous acid. Hypoiodous acid is a very strong anti microbial, with special activity against fungus. This is more evidence of Travis’s theory of potassium iodide as a strong anti fungal.
Potassium iodide is most certainly highly effective, it is also: safer, cheaper, and more available than synthetic azole constructs. This does not negatively-affect the thyroid, and you can even buy it from ebay.com.
Lehrer, R. I. "Antifungal effects of peroxidase systems." Journal of bacteriology (1969)
The reason the iodide ion (I⁻) works is likely because of the enzyme neutrophil myeloperoxidase, which converts in into the hypoiodite ion (IO⁻) using a hydrogen peroxide (H₂O₂) cosubstrate and a heme cofactor. The second greatest risk factor for candidiasis—and for all yeast & fungal infections in general—is neutropenia, or having low concentrations of circulating neutrophils. Studies on rats both consistently and plainly demonstrate the importance of neutrophils, and more elaborate genetic knockout studies prove myeloperoxase accounts for nearly all of this activity. Injections of only myeloperoxidase, the bare enzyme itself, have been shown to greatly enhance in vivo yeast killing potential and greatly promote survival.
Wright, C. D. "Candidacidal activity of myeloperoxidase: therapeutic influence of the enzyme in vivo." Infection and immunity (1985)
Although neutrophil myeloperoxidase can convert the more ubiquitous chloride ion (Cl⁻) into hypochlorite (ClO⁻) in an analogous manner: the iodide product is always shown more effective in in vitro combat assays, those pinning Neutrophils vs Fungi. Upon incubation with sodium or potassium iodide, yeast cell wall chitin has analytically been found iodinated after such neutrophil/fungi interactions—ostensibly by myeloperoxidase acting through a hypoiodide (IO⁻) intermediate. The efficacy of hypoiodide relative to the other hypohalide products (ClO⁻, BrO⁻, SCNO⁻) can be understood by noting: (1) hypoiodite is second only to hypothiocyanite (SCNO⁻) in oxidizing potential; (2) the kinetic rate of formation is the greatest for hypoiodide (IO⁻), meaning that more of this can be formed per unit time than any other; (3) iodide is most lipophilic of the group, enhancing its affinity for yeast cell membranes; (4) hypotiodite's conjugate acid has the highest Pka of the series, meaning that most will actually exist in the protonated hypoiodous acid form (HIO). [The neutral electronic charge of hypoiodous acid (HIO) means that it's the only hypohalide that is not repelled by the negatively-charged yeast cell membrane.] Thus: hypoiodous acid (HIO) is the most effective product of myeloperoxidase, the most effective enzyme against yeast that—in turn—also happens to be one secreted by the most effective immune cell type against same.
Lehrer, Robert I. "Leukocyte myeloperoxidase deficiency and disseminated candidiasis: the role of myeloperoxidase in resistance to Candida infection." The Journal of clinical investigation (1969)Aratani, Yasuaki. "Severe Impairment in Early Host Defense against Candida albicans in Mice Deficient in Myeloperoxidase." Infection and immunity (1999)Neutrophil myeloperoxidase has consistently been shown to enhance the survival of several species of small furry animals. These effects of course not limited to rodents, and potassium iodide—i.e. the preferred myeloperoxidase substrate—has clinically been used for human yeast/fungal infections for centuries. Potassium iodide is still used in countries having less pharmaceutical presence, and between 1–3 grams per day are often given with very few side effects; that observed in 5% of cases can be attributed to an increased concentration fungal 'die-off' metabolites. This certainly works in humans, and massive tumors of Basidiobolus haptosporus have been veritable dissolved in this manner:
Thotan, Sundeep Payyanur. "Subcutaneous Phycomycosis—Fungal Infection Mimicking a Soft Tissue Tumor: A Case Report and Review of Literature."Journal of tropical pediatrics (2009)
Even high doses do not appreciably effect thyroid hormone concentrations because the substantial volume of the extracellular space compartment, and iodide's (I⁻) natural affinity for it, prevents plasma iodide (I⁻) concentrations from undergoing large fluctuations. Iodide of course naturally ionically-associates with polysaccharides, perhaps why plasma levels remain stable after even gram-sized doses. Extracellular glycogen and fatty membranes act analogously to a 'buffer,' or a 'ballast,' in this scenario; toxicity only appears to occur at levels over 20 grams per day. And perhaps surprisingly, side effects from über-megadose KI has more to do with the potassium ion than with the iodide ion.
Utz, John. "Pulmonary aspergillosis with cavitation: iodide therapy associated with an unusual electrolyte disturbance." New England Journal of Medicine (1959)
This certainly shouldn't be viewed as a reason for avoidance; even sodium chloride can be fatal at 30 grams per day.
