AlphaCog
Member
- Joined
- Jan 28, 2014
- Messages
- 98
Beneficial Effects of a Low-Nickel Diet on Relapsing IBS-Like and Extraintestinal Symptoms of Celiac Patients during a Proper Gluten-Free Diet: Nickel Allergic Contact Mucositis in Suspected Non-Responsive Celiac Disease
Abstract
Background and aim: Nickel (Ni)-rich foods can induce allergic contact mucositis (ACM) with irritable bowel syndrome (IBS)-like symptoms in predisposed subjects. Ni ACM has a high prevalence (>30%) in the general population and can be diagnosed by a Ni oral mucosa patch test (omPT). Many celiac disease (CD) patients on a gluten-free diet (GFD) often show a recrudescence of gastrointestinal and extraintestinal symptoms, although serological and histological remission has been achieved. Since a GFD often results in higher loads of ingested alimentary Ni (e.g., corn), we hypothesized that it would lead to a consequent intestinal sensitization to Ni in predisposed subjects. We wanted to (1) study Ni ACM prevalence in still symptomatic CD patients on a GFD and (2) study the effects of a low-Ni diet (LNiD) on their recurrent symptoms.Material and methods: We recruited 102 consecutive CD patients (74 female, 28 male; age range 18-65 years, mean age 42.3 ± 7.4) on a GFD since at least 12 months, in current serological and histological remission (Marsh-Oberhuber type 0-I) who complained of relapsing gastrointestinal and/or extraintestinal symptoms.
Inclusion criteria: presence of at least three gastrointestinal symptoms with a score ≥5 on the modified Gastrointestinal Symptom Rating Scale (GSRS) questionnaire.
Exclusion criteria: IgE-mediated food allergy; history of past or current cancer; inflammatory bowel diseases; infectious diseases including Helicobacter pylori; lactose intolerance. All patients enrolled underwent Ni omPT and followed a LNiD for 3 months. A 24 symptoms questionnaire (GSRS modified according to the Salerno Experts' Criteria, with 15 gastrointestinal and 9 extraintestinal symptoms) was administered at T0 (free diet), T1 (GFD, CD remission), T2 (recurrence of symptoms despite GFD), and T3 (GFD + LNiD) for comparisons. Comparisons were performed using Wilcoxon signed-rank test.
Results: Twenty patients (all female, age range 23-65 years, mean age 39.1 ± 2.9) out of 102 (19.6%) were finally included. All 20 patients enrolled (100%) showed positive Ni omPT, confirming an Ni ACM diagnosis. A correct GFD (T0 vs. T1) induced the improvement of 19 out of the total 24 (79.2%) symptoms, and 14 out of 24 (58.3%) were statistically significant (p-value < 0.0083 according to Bonferroni correction). Prolonged GFD (T1 vs. T2) revealed the worsening of 20 out of the total 24 (83.3%) symptoms, and 10 out of 24 (41.7%) were statistically significant. LNiD (T2 vs. T3) determined an improvement of 20 out of the total 24 (83.4%) symptoms, and in 10 out of 24 (41.7%) symptoms the improvement was statistically significant.
Conclusions: Our data suggest that the recrudescence of gastrointestinal and extraintestinal symptoms observed in CD subjects during GFD may be due to the increase in alimentary Ni intake, once gluten contamination and persisting villous atrophy are excluded. Ni overload can induce Ni ACM, which can be diagnosed by a specific Ni omPT. Improvement of symptoms occurs after a proper LNiD. These encouraging data should be confirmed with larger studies.
Keywords: allergic contact mucositis; celiac disease; gluten-free diet; irritable bowel syndrome (IBS); low-nickel diet; nickel allergy; refractory celiac disease; remission.

Foods with high nickel (Ni) content and their possible overlap with foods rich in fermentable oligo-, di-, and monosaccharides and polyols (FODMAPs). Here we report some of the main foods belonging to specific categories. To be noted is the overlap between Ni-rich foods and foods with high FODMAP content, as well as the overlap between foods high in FODMAPs and lactose content.
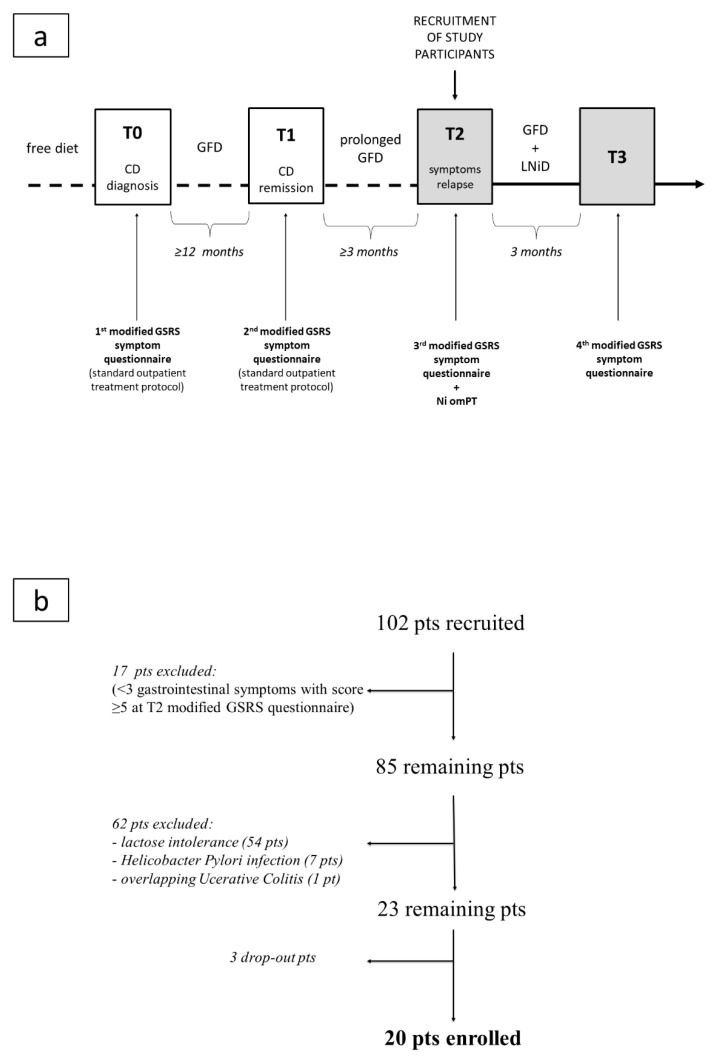
Flow charts of the study: (a) study arrangement; (b) patient enrollment. Legend: CD, celiac disease; GFD, gluten-free diet; GSRS, Gastrointestinal Symptom Rating Scale; LNiD, low-nickel diet; Ni omPT, nickel oral mucosa patch test; pts, patients.
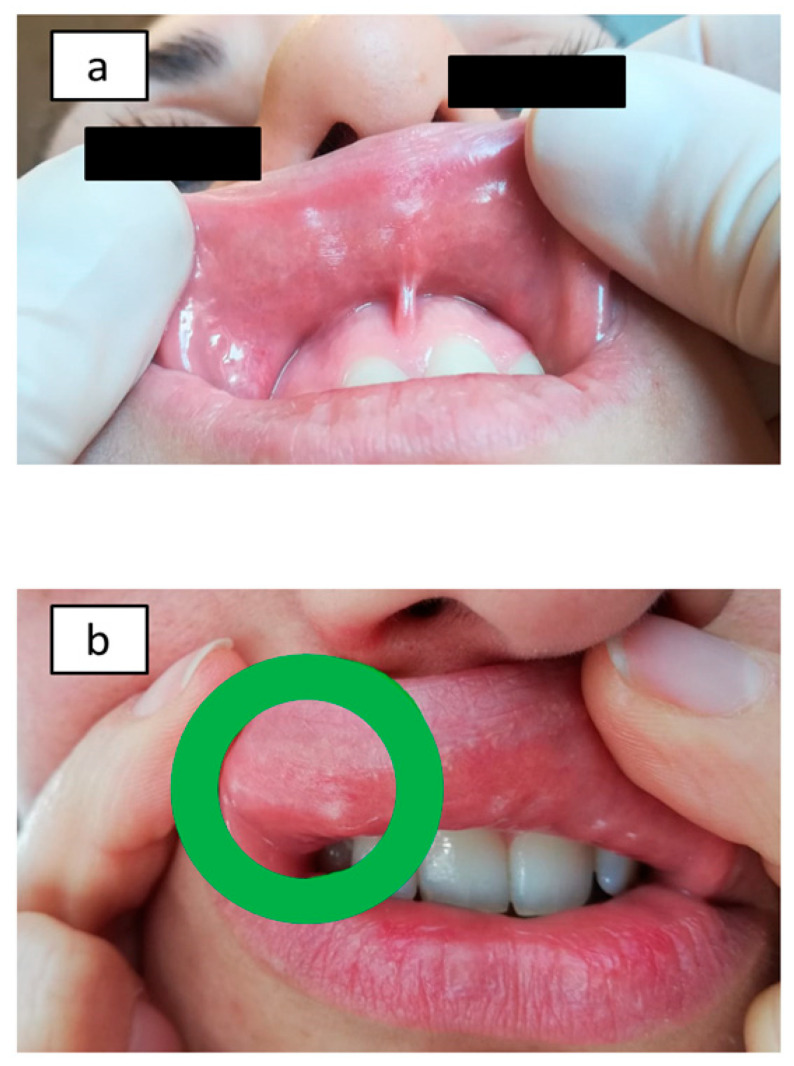
Nickel oral mucosa patch test (Ni omPT) results: Ni-sensitive patients before Ni omPT application (a) and after Ni omPT removal (2 h) (b).

Variation of gastrointestinal symptoms in celiac patients during different stages of the study. The p-value was calculated using the Wilcoxon signed-rank test (statistically significant p-value < 0.0083 according to Bonferroni correction). Legend: GSRS, Gastrointestinal Symptom Rating Scale; T0, baseline, during gluten-containing diet; T1, after ≥12 months of proper gluten-free diet; T2, after ≥3 months of prolonged gluten-free and Ni-rich diet; T3, after 3 months of low-nickel and gluten-free diet.

Variation of extraintestinal symptoms in celiac patients during different stages of the study. The p-value was calculated using the Wilcoxon signed-rank test (statistically significant p-value < 0.0083 according to Bonferroni correction). Legend: GSRS, Gastrointestinal Symptom Rating Scale; T0, baseline, during gluten-containing diet; T1, after ≥12 months of proper gluten-free diet; T2, after ≥3 months of prolonged gluten-free and nickel-rich diet; T3, after 3 months of low-nickel and gluten-free diet.

Beneficial Effects of a Low-Nickel Diet on Relapsing IBS-Like and Extraintestinal Symptoms of Celiac Patients during a Proper Gluten-Free Diet: Nickel Allergic Contact Mucositis in Suspected Non-Responsive Celiac Disease - PubMed
Our data suggest that the recrudescence of gastrointestinal and extraintestinal symptoms observed in CD subjects during GFD may be due to the increase in alimentary Ni intake, once gluten contamination and persisting villous atrophy are excluded. Ni overload can induce Ni ACM, which can be...
Last edited:
