tankasnowgod
Member
- Joined
- Jan 25, 2014
- Messages
- 8,131
Earlier this year, I started to think that the primary driver of Visceral Fat was probably from either an inflamed gut, a fatty liver, or both. So, I was pretty excited to come across this article from the Journal of Obesity that seems to posit the same thing. This article went a bit further, in suggesting that an inflamed gut likely causes fatty liver!
https://onlinelibrary.wiley.com/doi/full/10.1038/oby.2011.68
"Given the role of the gut in mesenteric fat inflammation and deposition and energy homeostasis, it is tempting to postulate that the gut is an important driving force for the pathophysiology of visceral obesity and its related metabolic disorders, in particular fatty liver diseases—thanks to the portal system. Similar gut‐liver interactions have been implicated as an important underlying mechanism by which alcoholic liver disease occurs (94). As summarized in Figure 1, it may all start with gut inflammation. As a consequence of alterations of gut microbiota composition and/or other external factors, gut barrier function is impaired and results in a “leaky gut.” The infiltration of microbial products into the mesenteric fat triggers an innate immune response and subsequently induces the production of proinflammatory cytokines from ATMs. The fat depot also expands as a protective mechanism to prevent the microbial antigens from further infiltrating the peritoneal cavity. Together these results in an increase flux of free‐fatty acids and proinflammatory factors, originating from both gut microbiota and the visceral fat depot, to the liver via the portal circulation.
When the availability of free‐fatty acids exceeds the capacity of both fat oxidation and triglyceride export as very‐low‐density lipoprotein, an excess of lipid accumulates in the liver. Subsequently, the increase in lipid derivatives (e.g., ceramide and diacylglycerol), together with proinflammatory factors from the portal circulation (95), activate inflammatory pathways in the liver. These events lead to common obesity‐associated liver diseases including nonalcoholic fatty liver disease and hepatic insulin resistance. The diseased liver, of course, leads to further metabolic abnormalities. Hepatic insulin resistance impairs the suppression of glucose production in the liver. Together with increased lipogenesis, the liver contributes to the elevated circulating levels of glucose and fatty acids that induce insulin secretion, elicit peripheral insulin resistance and eventually lead to a vicious cycle of metabolic dysfunction (96).
By the way, in case you are wondering what the Mesentary is-
The Mesentery - An Organ Of Interest
Personally, I think the two biggest drivers in this gut inflammation are the iron shavings added to wheat and rice, (thanks to so called "iron fortification" programs) and PUFAs, largely from vegetable oils. Adding in alcohol, especially beer, compounds this issue. Once the gut is compromised, other things that might be mostly benign or a small burden become a huge issue (all other starches, added gums, and high tryptophan foods like milk).
This leads me to believe my new focus on improving the gut barrier, reducing inflammation, and helping the liver is likely the way to go. It also makes me think that after certain offending items have been removed and enough time has been given to heal, that weight could come off very very quickly, even without a caloric deficit.
After all..... what if "visceral fat" isn't really "fat" at all? What if it's just water and inflammation?
https://onlinelibrary.wiley.com/doi/full/10.1038/oby.2011.68
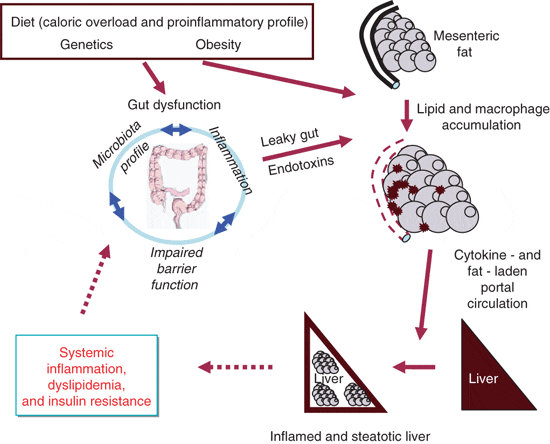
"Given the role of the gut in mesenteric fat inflammation and deposition and energy homeostasis, it is tempting to postulate that the gut is an important driving force for the pathophysiology of visceral obesity and its related metabolic disorders, in particular fatty liver diseases—thanks to the portal system. Similar gut‐liver interactions have been implicated as an important underlying mechanism by which alcoholic liver disease occurs (94). As summarized in Figure 1, it may all start with gut inflammation. As a consequence of alterations of gut microbiota composition and/or other external factors, gut barrier function is impaired and results in a “leaky gut.” The infiltration of microbial products into the mesenteric fat triggers an innate immune response and subsequently induces the production of proinflammatory cytokines from ATMs. The fat depot also expands as a protective mechanism to prevent the microbial antigens from further infiltrating the peritoneal cavity. Together these results in an increase flux of free‐fatty acids and proinflammatory factors, originating from both gut microbiota and the visceral fat depot, to the liver via the portal circulation.
When the availability of free‐fatty acids exceeds the capacity of both fat oxidation and triglyceride export as very‐low‐density lipoprotein, an excess of lipid accumulates in the liver. Subsequently, the increase in lipid derivatives (e.g., ceramide and diacylglycerol), together with proinflammatory factors from the portal circulation (95), activate inflammatory pathways in the liver. These events lead to common obesity‐associated liver diseases including nonalcoholic fatty liver disease and hepatic insulin resistance. The diseased liver, of course, leads to further metabolic abnormalities. Hepatic insulin resistance impairs the suppression of glucose production in the liver. Together with increased lipogenesis, the liver contributes to the elevated circulating levels of glucose and fatty acids that induce insulin secretion, elicit peripheral insulin resistance and eventually lead to a vicious cycle of metabolic dysfunction (96).
By the way, in case you are wondering what the Mesentary is-
The Mesentery - An Organ Of Interest
Personally, I think the two biggest drivers in this gut inflammation are the iron shavings added to wheat and rice, (thanks to so called "iron fortification" programs) and PUFAs, largely from vegetable oils. Adding in alcohol, especially beer, compounds this issue. Once the gut is compromised, other things that might be mostly benign or a small burden become a huge issue (all other starches, added gums, and high tryptophan foods like milk).
This leads me to believe my new focus on improving the gut barrier, reducing inflammation, and helping the liver is likely the way to go. It also makes me think that after certain offending items have been removed and enough time has been given to heal, that weight could come off very very quickly, even without a caloric deficit.
After all..... what if "visceral fat" isn't really "fat" at all? What if it's just water and inflammation?

