OP
extremecheddar
Member
- Joined
- Jan 2, 2014
- Messages
- 201
I also attribute much of my improvement to those two supplements specifically. I ran out of biotin, need to buy more.
Follow along with the video below to see how to install our site as a web app on your home screen.
Note: This feature may not be available in some browsers.
Click Here if you want to upgrade your account
If you were able to post but cannot do so now, send an email to admin at raypeatforum dot com and include your username and we will fix that right up for you.
RBTI has helped me tremendously...just stick to the basics, moderate breakfast, big lunch, small dinner. 3 meals a day.
Looks like this might be the trick I was looking for...
Looks like this might be the trick I was looking for...
Our laboratory is interested in the metabolic response to ingested proteins, particularly in persons with type 2 diabetes. The reason for this interest is that ingested protein either results in no increase in peripheral blood glucose concentrations or increases them only modestly (1, 2). However, ingested protein stimulates both insulin and glucagon secretion. In addition, in persons with type 2 diabetes, protein ingested with glucose reduces the integrated, single-meal glucose area response when compared with that after the ingestion of only glucose by the same subjects. This is due to a synergistic stimulation of insulin secretion when protein is ingested simultaneously with glucose (3).
Of 7 different protein sources tested previously, one of the most potent was gelatin (4). This was somewhat surprising because gelatin is an atypical protein. On a molar basis, glycine makes up ≈30% of the total amino acids present (5). Therefore, we were interested in determining whether glycine itself stimulates insulin secretion or reduces the integrated glucose response when ingested with a standardized amount of glucose. We first determined the response in normal young subjects.
The dramatic reduction in the glucose area response when glycine was ingested with glucose is of considerable interest from a physiologic point of view. However, the mechanism remains to be determined. The integrated insulin area response after the ingestion of glycine + glucose was essentially the same as when only glucose was ingested, but it occurred at a greatly attenuated increase in glucose concentration and without a delay in the return of the glucose concentration to the initial fasting value. This result is similar to that we and others observed in healthy subjects when fat was ingested with glucose (20, 21). It suggests that the glucose clearance rate was accelerated. The clearance rate of ingested glucose was not determined in any of these studies. Therefore, whether the attenuated increase in glucose and rapid return to the fasting value was due to 1) an increased removal rate either directly or indirectly as a result of the rise in insulin, 2) an independent mechanism, or 3) a decrease in the endogenous glucose production rate cannot be determined.
A decrease in the glucose production rate would not be expected in the presence of a persistent large increase in the glucagon concentration. In fact, one would anticipate an increase in glucose production. A reduction in the glucose absorption rate also is unlikely but cannot be ruled out. Glycine has been reported to compete with glucose for absorption (22). Cholecystokinin and glucagon-like peptide 1 (GLP-1,7-36 amide) strongly reduce the rate of gastric emptying. The latter hormone also may reduce duodenal motility (23). Intraduodenal instillation of a mixture of nutritionally required amino acids stimulates cholecystokinin secretion; individually, phenylalanine, valine, and methionine were most potent. Nonnutritionally required amino acids including glycine did not stimulate cholecystokinin secretion (24). GLP-1 also stimulates insulin secretion and reduces glucagon secretion. Because glycine stimulated an increase in both insulin and glucagon, a glycine-stimulated increase in GLP-1 is not likely to explain the results (23). Overall, the data suggest that oral glycine stimulates the secretion, either directly or indirectly, of a gut hormone that potentiates or is additive with the effect of insulin in stimulating the removal of glucose from the circulation. It also inhibits the effect of glucagon on endogenous glucose production. Nevertheless, this remains only a speculation at present.
In any regard, the ingested glycine effect on the postprandial glucose concentration may be important therapeutically if a similar effect can be shown in persons with type 2 diabetes. It will also be of interest to determine whether glycine synergistically facilitates insulin secretion by other amino acids that are quantitatively prominent in gelatin protein.
I'll try this for my reactive hypoglycemia, thanks for posting. I've recently been taking 10g of glycine powder before bed and it's significantly improved my sleep.
I have been taking 3 tbs Great Lakes Collagen before bed lately, and it improved my sleep remarkably.
Now I plan to experiment with taking glycine just before my meals as well. Isn't glycine way cheeper then collagen?
What a great post thank you @DuggaDugga.I saw this earlier today. I was curious why glycine had that effect, so I went looking. . . .
Well, as most of us are aware protein stimulates the secretion of insulin, but not all amino acids are created equally in that regard apparently.
The metabolic response to ingested glycine
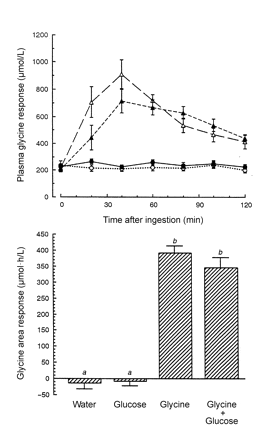
First, the glycine response seemed to be slightly attenuated by consumption with glucose with glycine.
But there's more to this story, since consumption of protein alone will stimulate, not just insulin, but also glucagon to antagonize the insulin. If it didn't the insulin would cause a precipitous drop in blood sugar. No bueno. We'll be back to that. . . .

Top: Mean (± SEM) plasma glycine response in 9 healthy subjects after the ingestion of water only (○….○), 25 g glucose (•––•), 1 mmol glycine/kg lean body mass (▵– –▵), or 25 g glucose + 1 mmol glycine/kg lean body mass (▴——▴). Bottom: The 120-min net integrated glycine area response with the use of the concentration at time zero as baseline. n = 9. Bars with different letters are significantly different, P ≤ 0.01.
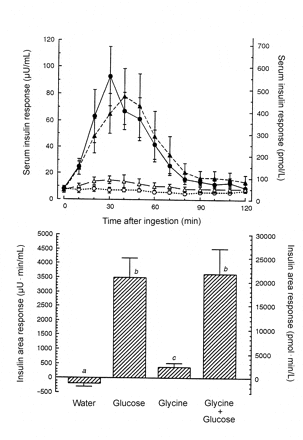
Second, we see that the insulin response was also attenuated by consumption of glycine with glucose.

Top: Mean (± SEM) serum insulin response in 9 healthy subjects after the ingestion of water only (○….○), 25 g glucose (•––•), 1 mmol glycine/kg lean body mass (▵– –▵), or 25 g glucose + 1 mmol glycine/kg lean body mass (▴——▴). Bottom: The 120-min net integrated insulin area response with the use of the concentration at time zero as baseline. n = 9. Bars with different letters are significantly different, P ≤ 0.01.
After a cursory review, it appears that the two buffer the metabolism of one another like Chris mentioned.
Back to glucagon. . . .

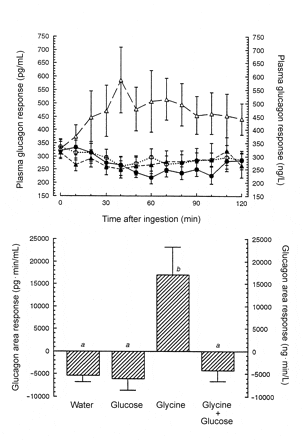
Top: Mean (± SEM) plasma glucagon response in 9 healthy subjects after the ingestion of water only (○….○), 25 g glucose (•––•), 1 mmol glycine/kg lean body mass (▵– –▵), or 25 g glucose + 1 mmol glycine/kg lean body mass (▴——▴). Bottom: The 120-min net integrated glucagon area response with the use of the concentration at time zero as baseline. n = 9. Bars with different letters are significantly different, P ≤ 0.01.
Look at the differences! Glycine alone caused a massive spike in glucagon, while consumption of glycine with carbs or carbs alone had no such effect. Makes sense. The body knows it glucose to use with the insulin, so it wants to keep us sensitive to it. No risk of blood sugar plummeting
Next (and what I think is the most important), is the proposed mechanism. . . .
The proposed reasoning is the release of peptide hormones that slow digestion and promote the secretion of digestive enzymes and bile. Possibly, this is why Ray recommends eating saturated fats to slow the digestion of starches to attenuate spikes in blood sugar. Though through different mechanisms, we might consider the advantage of consuming food with fructose to potentiate insulin secretion to also help moderate blood glucose.
Sweet taste receptor signaling in beta cells mediates fructose-induced potentiation of glucose-stimulated insulin secretion. - PubMed - NCBI
Eating only fruit, juice, dairy, sugar, and non starchy vegetables for carbs does give me hypoglycemia issues after about 2 weeks on a no starch diet.