Tristan Loscha
Member
- Joined
- Dec 18, 2018
- Messages
- 2,206
The impact of a vegan diet on pregnancy outcomes
Tomer Avnon 1,2 ● Efrat Paz Dubinsky3 ● Inbar Lavie2 ● Tali Ben-Mayor Bashi1 ● Ronit Anbar3,4 ● Yariv Yogev1,2
Received: 21 April 2020 / Revised: 28 July 2020 / Accepted: 25 August 2020
© The Author(s), under exclusive licence to Springer Nature America, Inc. 2020
Abstract
Objective To determine the effect of a maternal vegan diet on pregnancy outcome.
Study design This is a prospective observational study. Women with a singleton pregnancy who maintained the same diet
prior to, and throughout current pregnancy were enrolled. Stratification was performed according to diet type: vegans,
lacto–ovo–vegetarians, fish-eaters, and omnivores.
Results Overall, 273 women were enrolled, of them, 112 omnivores, 37 fish-eaters, 64 lacto–ovo–vegetarians, and 60
vegans. The vegan diet was significantly associated with an increased risk of small-for-gestational-age newborns compared
only to an omnivore diet (RR = 5.9, 95% CI, 1.2–21.8). The incidence of preterm birth was similar in all groups. Vegans
had lower birthweight compared to lacto–ovo–vegetarians (3015 ± 420 g vs. 3285 ± 482 g, P = 0.004), and to omnivores
(3328 ± 495 g, P < 0.001), but not to fish-eaters. Vegans also had a lower mean gestational weight gain compared only to
omnivores (11.6 ± 4.2 kg vs. 14.3 ± 4.6 kg, P = 0.001).
Conclusion The vegan diet is associated with an increased risk for small-for-gestational-age newborns and lower
birthweight.
Journal of Perinatology
https://doi.org/10.1038/s41372-020-00804-x
ARTICLE
The impact of a vegan diet on pregnancy outcomes
Tomer Avnon 1,2 ● Efrat Paz Dubinsky3 ● Inbar Lavie2 ● Tali Ben-Mayor Bashi1 ● Ronit Anbar3,4 ● Yariv Yogev1,2
Received: 21 April 2020 / Revised: 28 July 2020 / Accepted: 25 August 2020
© The Author(s), under exclusive licence to Springer Nature America, Inc. 2020
Abstract
Objective To determine the effect of a maternal vegan diet on pregnancy outcome.
Study design This is a prospective observational study. Women with a singleton pregnancy who maintained the same diet
prior to, and throughout current pregnancy were enrolled. Stratification was performed according to diet type: vegans,
lacto–ovo–vegetarians, fish-eaters, and omnivores.
Results Overall, 273 women were enrolled, of them, 112 omnivores, 37 fish-eaters, 64 lacto–ovo–vegetarians, and 60
vegans. The vegan diet was significantly associated with an increased risk of small-for-gestational-age newborns compared
only to an omnivore diet (RR = 5.9, 95% CI, 1.2–21.8). The incidence of preterm birth was similar in all groups. Vegans
had lower birthweight compared to lacto–ovo–vegetarians (3015 ± 420 g vs. 3285 ± 482 g, P = 0.004), and to omnivores
(3328 ± 495 g, P < 0.001), but not to fish-eaters. Vegans also had a lower mean gestational weight gain compared only to
omnivores (11.6 ± 4.2 kg vs. 14.3 ± 4.6 kg, P = 0.001).
Conclusion The vegan diet is associated with an increased risk for small-for-gestational-age newborns and lower
birthweight.
Introduction
The number of people who choose to maintain a vegan or
lacto–ovo–vegetarian (LOV) diet and abstain from any
animal-based food has steadily increased over the past few
years. A vegan diet is distinguished from a LOV diet by
being limited to plant-based products and the omission of
dairy products and eggs [1]. Since a vegan diet is different
from LOV diet, it may potentially lead to other nutritional
deficits, depending on supplementation intake, including
vitamins B12 [1–8], B2 [3], and D [4, 5, 7], calcium [5, 7],
iron, zinc [5], and even iodine [6]. The maternal diet during
pregnancy has a direct effect on the newborn’s metabolism,
such as impaired bone mass, during childhood [9], while
low maternal B12 levels associates with insulin resistance,
and changes in lipid profile ratio in the umbilical cord [10].
Few studies have examined the effect of a vegan diet on
pregnancy outcome [11–13]. Although some of them
showed a positive association between birthweight and
maternal consumption of mainly plant-based foods [7, 12],
those studies focused on LOV or on women in the general
population, and not on the vegan population. The data on
the impact of LOV and vegan diets on the gestational age at
delivery, the incidence of preterm delivery [11], as well as
on birthweight [7, 11–15], are inconsistent. The mentioned
studies were performed in different countries with heterogenous
social, cultural, and dietary patterns, which could
influence and cause inconsistent results. In addition, since
vegan women are reportedly at risk of deficiencies of various
vitamin levels, such as B12 and D, their newborns may
also sustain similar deficiencies [8, 11, 12].
In this study, we aimed to determine the association
between specific maternal diet and pregnancy outcome,
especially intrauterine growth restriction and preterm birth,
by comparing women who followed vegan diet to women
who followed lacto–ovo–vegetarian, fish-eaters, and omnivore
diets.
* Tomer Avnon
[email protected]
1 Department of Obstetrics & Gynecology, Lis Maternity &
Women’s Hospital, Tel-Aviv Sourasky Medical Center, affiliated
to the Sackler Faculty of Medicine, Tel-Aviv University,
Tel-Aviv, Israel
2 Sackler Faculty of Medicine, Tel-Aviv University, Tel-Aviv, Israel
3 Nutrition and Dietetic Unit, Tel-Aviv Sourasky Medical Center,
affiliated to the Sackler Faculty of Medicine, Tel-Aviv University,
Tel-Aviv, Israel
4 School of Nutritional Sciences, The Robert H Smith Faculty of
Agriculture, Food and Environmental Quality Sciences, Hebrew
University, Jerusalem, Israel
1234567890();,:
1234567890();,:
Methods
Study population
This prospective observational study of women who gave
birth at a tertiary, university-affiliated medical center was
conducted between May 2018 and June 2019. Eligibility
was limited to women aged 18 years or more with a singleton
pregnancy. Only women who maintained the same
diet for at least 3 months prior to and throughout the current
pregnancy were enrolled. The exclusion criteria were a prior
medical indication for a specific restrictive diet, such as pregestational
diabetes mellitus, celiac disease, lactose intolerance,
and inflammatory bowel disease, and having
undergone bariatric procedures or other bowel resections.
The women were divided into four categories according to
their diet: vegans, who consume only plant-based products,
LOV, who consume mainly plant-based products but also
dairy products and eggs, fish-eaters, who include fish products
in their LOV diet, and omnivores, who consume
animal-based and plant-based products. All the participants
were asked to fill in questionnaires on a diet they followed
throughout their pregnancy. We did not offer any dietary
consultation to prevent interference with the results. The
average caloric and protein intake were for vegans 1984.73 ±
734.91 kcal/day and 59.85 ± 24.15 g/day, for LOV 1773.30 ±
598.90 kcal/day and 60.46 ± 20.71 g/day, for fish-eaters
1809.89 ± 434.03 kcal/day and 68.56 ± 25.19 g/day, and
for omnivores 1733.73 ± 514.45 kcal/day and 78.21 ±
30.95 g/day, respectively. We did not exclude women based
on consumption or not of vitamin supplementation, though
most of the women in all of the diet groups consumed vitamin
supplementation. We recently published that the levels of
vitamin B12 and ferritin levels are similar between pregnant
vegans to LOV and omnivores. Furthermore, we demonstrated
that pregnant vegans who do not consume vitamin
supplementation have lower B12 levels, but still within the
normal range [16].
Data were extracted from the real-time computerized
database and from the filled-in questionnaires. The items
included: eating habits and length of following a specific
diet, maternal age, gravidity, parity, medical information,
vitamins and supplementations taken, body mass index
(BMI) at the time of conception and gestational weight gain
during pregnancy, mode of conception (either spontaneous
or artificial reproductive techniques), mode of delivery, and
gestational age at delivery. Maternal complications included
gestational diabetes mellitus (GDM), defined according to
the American College of Obstetrics and Gynecologists
(ACOG) definitions [17], preeclampsia (PE) and gestational
hypertension, defined according to ACOG definitions [18],
postpartum hemorrhage (PPH), and presence of meconium.
The recorded neonatal information included birthweight and
the 5-min Apgar score. The mean birth percentile for each
neonate was adjusted for gender and gestational age at
delivery according to local population birth curve percentiles
[19]. Primary outcomes were preterm birth (delivery
prior to 37 weeks) and incidence of small-for-gestationalage
(SGA: birthweight below the 10% percentile). Secondary
outcomes were birthweight, the incidence of GDM,
PE, and gestational hypertension, mode of delivery, PPH,
gestational weight gain, and a 5-min Apgar score below 7.
The local institutional review board approved the study
(0715-17-TLV), and all women provided written informed
consent.
Data analysis
Descriptive statistics of demographic and clinical characteristics
were generated by the type of diet followed
during pregnancy. Differences between the selected parameters
of the four study groups were evaluated by one-way
ANOVA and chi-square tests. A hierarchical linear regression
model was used to predict neonatal birthweight and
maternal gestational weight gain among vegans compared
to LOV, fish-eaters, and omnivores, adjusted for maternal
age and BMI. A hierarchical logistic regression model was
used to predict SGA among the neonates of the vegan
mothers compared to the other mothers, adjusted for
maternal age and BMI. Based on the regression model diet
Exp(B) coefficient, we calculated an adjusted relative risk
(RR) for the neonates of vegan mothers to be SGA compared
to the other neonates [20]. A P value of 0.05 was
considered statistically significant. Statistical analysis was
performed with IBM SPSS statistics version 26.
Results
Of the 273 women enrolled in this study, 112 were omnivores,
37 were fish-eaters, 64 were LOV, and 60 were
vegans. The demographic characteristics of the study cohort
are provided in Table 1. The vegan women were older and
had a significantly lower pre-gestational BMI in comparison
to the other groups.
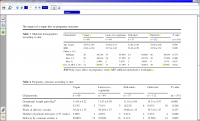
Pregnancy outcomes are provided in Table 2. The
omnivores had the lowest incidence of SGA newborns
(1.79%), and vegans had the highest incidence of SGA
newborns (11.67%, RR = 5.93, 95% CI, 1.20–21.83).
Adjustment for maternal age and pre-pregnancy BMI was
performed due to the demographic differences between
the four groups. The incidence of SGA newborns among the
vegans remained significantly higher compared to the
newborns of the omnivores (95% CI, 0.03–0.71, P =
T. Avnon et al.
0.018), but not compared to the newborns of the LOV (95%
CI, 0.11–1.70, P = 0.236) or fish-eaters (95% CI,
0.25–3.70, P = 0.965). The incidence of preterm birth was
similar in all groups (P = 0.888).
After adjustment for maternal age and pre-pregnancy
BMI, there was a significant difference in neonatal birthweight
between the groups (P = 0.002). The neonatal
birthweight for the vegan group was lower than that for the
LOV group (3015 ± 420 g vs. 3285 ± 482 g, 95% CI,
86.01–440.36, P = 0.004) and that for the omnivore group
(3328 ± 495 g, 95% CI, 142.21–459.34, P < 0.001), but not
for the fish-eaters group (3175 ± 463 g, 95% CI −48.04 to
357.84, P = 0.134); although all mean birthweights were
within the normal range for the local population. After
adjustment for maternal age and pre-pregnancy BMI,
gestational weight gain was significantly different between
the groups (P < 0.001): the vegans had a significantly lower
gestational weight gain in comparison to the omnivores
(11.6 ± 4.2 kg vs. 14.3 ± 4.6 kg, 95% CI, 1.13–4.10, P =
0.001), but not to the fish-eaters (11.2 ± 3.8 kg, 95% CI,
−2.36 to 1.41, P = 0.622), or to the LOV (11.97 ± 4.6 kg,
95% CI, −1.20 to 2.12, P = 0.588).
There was no significant difference between the groups
for the incidence of hypertensive complications of pregnancy
(P = 0.865), GDM (P = 0.546), or cesarean sections
(P = 0.065).
During pregnancy, 30 women received nutritional consultation
(vegans 13.33%, LOV 6.25%, fish-eaters 10.81%,
and omnivores 12.50%). We did not find any influence for
nutritional consultation during pregnancy on any of the
measured outcomes.
Discussion
We aimed to determine the influence on pregnancy outcomes
of the vegan diet in comparison to fish-eaters and
omnivore diets. Our main findings were:
Table 2 Pregnancy outcome according to diet.
Vegan Lacto–ovo–
vegetarian
Fish-eaters Omnivore P value
Characteristic n = 60 n = 64 n = 37 n = 112 (α = 5%)
Gestational weight gain (Kg)# 11.65 ± 4.22 11.97 ± 4.59 11.18 ± 3.84 14.31 ± 4.57 <0.001
GDM, n 8.33% 5 7.81% 5 16.22% 6 8.93% 10 0.546
Week of delivery (weeks) 39.24 ± 1.72 39.49 ± 1.57 39.68 ± 1.33 39.72 ± 1.47 0.237
Number of preterm deliveries (<37 weeks) 5.00% 3 4.69% 3 5.41% 2 3.57% 4 0.888
Delivery by cesarean section, n 20.00% 12 25.00% 16 8.11% 3 12.50% 14 0.065
Hypertensive complications, n 3.33% 2 3.13% 2 2.70% 1 1.79% 2 0.865
Postpartum hemorrhage, n 5.00% 3 9.38% 6 13.51% 5 8.93% 10 0.537
5-min Apgar score ≤7, n 0.00% 0 1.56% 1 0.00% 0 0.00% 0 0.866
Average birthweight (g)# 3015.2 ± 420.4 3285.1 ± 482.3 3175.1 ± 463.4 3328 ± 495.8 0.002
Low birthweight (<2500 g), n 11.67% 0 7.81% 5 8.11% 3 3.57% 4 0.198
Number of SGA (<10%)# 11.67% 7 6.25% 4 10.81% 4 1.79% 2 0.021
Number of SGA (<10%)# P value = 0.236 P value = 0.965 P value = 0.018
Vegan compared to other diet groups.
#Adjusted to age and body mass index (BMI) at pregnancy onset.
GDM gestational diabetes mellitus, SGA small-for-gestational-age.
Table 1 Maternal demographics
according to diet.
Characteristic Vegan Lacto–ovo–vegetarian Fish-eaters Omnivore P value
n= 60 n = 64 n = 37 n = 112 (α = 5%)
Age (years) 34.97 ± 3.85 33.56 ± 4.13 32.62 ± 3.63 32.56 ± 4.02 0.010
BMI 21.41 ± 2.63 23.51 ± 3.42 21.82 ± 2.93 22.56 ± 3.32 0.020
Parity, n (%)
Nullipara 29 48.33% 35 54.69% 24 64.86% 66 58.93% 0.374
Para 1–2 28 46.67% 24 37.50% 11 29.73% 42 37.50% 0.400
Para 3+ 3 5.00% 5 7.81% 2 5.40% 4 3.57% 0.637
Use of ART, n (%) 12 20.0% 11 17.19% 4 10.81% 10 8.93% 0.162
BMI body mass index at pregnancy onset, ART artificial reproductive techniques.
The impact of a vegan diet on pregnancy outcomes
1. Vegans had an increased risk for SGA neonates in
comparison to omnivores and lower mean birthweight
neonates, though within the normal range, in
comparison to omnivores and LOV. In addition,
vegans had lower gestational weight gain in comparison
to omnivores.
2. No difference was found between the four diet groups
for the incidence of hypertensive complications,
GDM, or preterm birth.
Our finding of a lower birthweight among the neonates
of vegans compared to the neonates of omnivores and LOV
are supported by the findings of Ferrara et al. [13] but
apposed conflicting results by others. In the study of Tan
et al. [15], LOV diet did not demonstrate any effect on
birthweight, while Piccoli et al. [11] mentioned heterogenous
birthweights among LOV. Sebastiani et al. [7]
reported a positive relationship between fruit and vegetable
consumption to birthweight, but their study did not specifically
refer to a diet which is completely derived from any
animal-based products. Furthermore, our study is the first to
show a significantly higher incidence of SGA neonates
among vegans, and that the risk remained significant even
after adjustment for maternal age and pre-pregnancy BMI.
Our findings are in agreement with those of Zulyniak et al.
[14], which demonstrated a higher incidence of SGA among
women who consume a plant-based diet, although, like
many other earlier studies, they did not isolate the vegan
population.
Vegans are usually leaner than omnivores [21], and the
vegans in our study also gained less weight during pregnancy
compared to omnivores. This difference might
mediate the lower birthweight among the vegan neonates,
given that women who gain less weight than recommended
are reportedly at risk for having smaller children [22, 23]. It
would follow, therefore, that consulting vegans to aim for
an adequate gestational weight gain might lower that
increased risk for SGA neonates.
We did not find any difference between diet groups in the
duration of pregnancy or in the risk for preterm birth, which
is in agreement with others [11]. We also did not find any
relationship between the vegan diet to hypertensive complications
of pregnancy (either preeclampsia or gestational
hypertension), unlike one previous study that showed a
lower risk among vegans [24]. There is a known association
between increased BMI and prevalence of GDM [25].
While some studies demonstrated a lower risk for GDM
among LOV [7, 26], or mixed results [15], to the best of our
knowledge, no other study has related specifically to the
influence of a vegan diet on the risk for GDM, which we
found to have any effect.
We demonstrated that vegans have an increased risk for
lower neonatal birthweight, albeit within the normal range.
We also found that they had an increased risk for SGA
neonates and for lower gestational weight gain and hypothesized
that the latter might mediate the birthweight differences.
Therefore, we think that our findings should not be
used to persuade vegans to abandon their diets, but rather
that they be encouraged to maintain a healthy diet and to
undergo regular follow-up of maternal weight and fetal
weight estimation and to undergo specific diet consultation.
The strengths of our study are that it is one of the largest
on pregnancy outcomes that focused specifically on the
vegan population. Unlike many past studies that combined
vegans and LOV, or that had only a few vegan patients, our
study differentiated them from LOV in the evaluations of all
the selected parameters. We prevented contamination of the
results by restricting the study to women who followed the
same diet for at least 3 months prior to their pregnancy up to
delivery. We also recruited women during different stages
of their pregnancy in order to maintain heterogenicity and to
prevent selection bias.
Our study has some limitations that bear mention.
Although it is one of the largest studies of its kind, we were
not able to stratify other demographic characteristics, such
as education, alcohol consumption, and smoking. We also
excluded women who began their pregnancy while following
a vegan or LOV diet and changed it during the
course of pregnancy. Thus, precluding our ability to determine
whether there is a specific point in pregnancy in which
a change in diet might influence the outcomes.
Our findings suggest that a vegan diet is associated with
an increased risk for SGA and lower-birthweight neonates
and with lower gestational weight gain. Vegan women
should be encouraged to maintain a healthy diet, consult a
dietician, followed regularly for fetal growth, including
sonographic screening for intrauterine growth restriction
and followed for adequate gestational weight gain during
their pregnancy.
Funding No funding was received.
Author contributions Tomer Avnon—conception, methodology,
investigation supervision, data curation, formal analysis, and drafting
the initial paper. Efrat Paz Dubinsky—investigation and data curation.
Inbar Lavie—formal analysis. Tali Ben-Mayor Bashi—investigation
and data curation. Ronit Anbar—methodology and investigation.
Yariv Yogev—methodology, investigation supervision, and resources.
All authors revised the paper, gave final approval of the version to be
published, and agreed to be accountable for all aspects of the work.
Compliance with ethical standards
Conflict of interest The authors declare that they have no conflict of
interest.
Publisher’s note Springer Nature remains neutral with regard to
jurisdictional claims in published maps and institutional affiliations.
T. Avnon et al.
References
1. Key TJ, Appleby PN, Rosell MS. Health effects of vegetarian and
vegan diets. Proc Nutr Soc. 2006;65:35–41.
2. Gilsing AMJ, Crowe FL, Lloyd-Wright Z, Sanders TAB, Appleby
PN, Allen NE, et al. Serum concentrations of vitamin B12 and
folate in British male omnivores, vegetarians and vegans: results
from a cross-sectional analysis of the EPIC-Oxford cohort study.
Eur J Clin Nutr. 2010;64:933–9.
3. Majchrzak D, Singer I, Männer M, Rust P, Genser D, Wagner KH,
et al. B-vitamin status and concentrations of homocysteine in
Austrian omnivores, vegetarians and vegans. Ann Nutr Metab.
2007;50:485–91.
4. Elorinne AL, Alfthan G, Erlund I, Kivimäki H, Paju A, Salminen
I, et al. Food and nutrient intake and nutritional status of Finnish
vegans and non-vegetarians. PLoS ONE. 2016;11:1–14.
5. Winston CJ. Health effeets of vegan diets 1-3. Am J Clin Nutr.
2009;89:1627–33.
6. Leung AM, LaMar A, He X, Braverman LE, Pearce EN. Iodine
status and thyroid function of Boston-area vegetarians and vegans.
J Clin Endocrinol Metab. 2011;96:1303–7.
7. Sebastiani G, Barbero AH, Borrás-Novel C, Casanova MA,
Aldecoa-Bilbao V, Andreu-Fernández V, et al. The effects of
vegetarian and vegan diet during pregnancy on the health of
mothers and offspring. Nutrients. 2019;11:1–29.
8. Pawlak R. To vegan or not to vegan when pregnant, lactating or
feeding young children. Eur J Clin Nutr. 2017;71:1259–62.
9. Ganpule A, Yajnik CS, Fall CHD, Rao S, Fisher DJ, Kanade A,
et al. Bone mass in Indian children—relationships to maternal
nutritional status and diet during pregnancy: the Pune maternal
nutrition study. J Clin Endocrinol Metab. 2006;91:2994–3001.
10. Adaikalakoteswari A, Vatish M, Lawson A, Wood C, Sivakumar
K, McTernan PG, et al. Low maternal vitamin B12 status is
associated with lower cord blood HDL cholesterol in white caucasians
living in the UK. Nutrients. 2015;7:2401–14.
11. Piccoli GB, Clari R, Vigotti FN, Leone F, Attini R, Cabiddu G,
et al. Vegan-vegetarian diets in pregnancy: danger or panacea? A
systematic narrative review. BJOG Int J Obstet Gynaecol.
2015;122:623–33.
12. Pistollato F, Sumalla Cano S, Elio I, Masias Vergara M, Giampieri
F, Battino M. Plant-based and plant-rich diet patterns during
gestation: beneficial effects and possible shortcomings. Adv Nutr.
2015;6:581–91.
13. Ferrara P, Sandullo F, Di Ruscio F, Franceschini G, Peronti B,
Blasi V, et al. The impact of lacto-ovo-/lacto-vegetarian and vegan
diets during pregnancy on the birth anthropometric parameters of
the newborn. J Matern Neonatal Med. 2019;0:1–7.
14. Zulyniak MA, De Souza RJ, Shaikh M, Desai D, Lefebvre DL,
Gupta M, et al. Does the impact of a plant-based diet during
pregnancy on birth weight differ by ethnicity? A dietary pattern
analysis from a prospective Canadian birth cohort alliance. BMJ
Open. 2017;7:1–9.
15. Tan C, Zhao Y, Wang S. Is a vegetarian diet safe to follow during
pregnancy? A systematic review and meta-analysis of observational
studies. Crit Rev Food Sci Nutr. 2019;59:2586–96.
16. Avnon T, Anbar R, Lavie I, Ben-Mayor Bashi T, Paz Dubinsky E,
Shaham S, et al. Does vegan diet influence umbilical cord vitamin
B12, folate, and ferritin levels? Arch Gynecol Obstet.
2020;301:1417–22.
17. Committee on Practice Bulletins—Obstetrics. ACOG Practice
Bulletin No. 190: Gestational diabetes mellitus. Obstet Gynecol.
2018;131;e49–64.
18. Committee on Practice Bulletins—Obstetrics. ACOG Practice
Bulletin No. 202: Gestational hypertension and preeclampsia.
Obstet Gynecol. 2019;133:e1–25.
19. Dollberg S, Haklai Z, Mimouni FB, Gorfein I, Gordon E-S. Birth
weight standards in the live-born population in Israel. Isr Med
Assoc J. 2005;7:311–4.
20. Zhang J, Yu KF. What’s the relative risk? A method of correcting
the odds ratio in cohort studies of common outcomes. J Am Med
Assoc. 1998;280:1690.
21. Rosell M, Appleby P, Spencer E, Key T. Weight gain over 5 years
in 21 966 meat-eating, fish-eating, vegetarian, and vegan men and
women in EPIC-Oxford. Int J Obes. 2006;30:1389–96.
22. Goldstein RF, Abell SK, Ranasinha S, Misso M, Boyle JA, Black
MH, et al. Association of gestational weight gain with maternal
and infant outcomes: a systematic review and meta-analysis. J Am
Med Assoc. 2017;317:2207–25.
23. Viswanathan M, Siega-Riz AM, Moos MK, Deierlein A, Mumford
S, Knaack J, et al. Outcomes of maternal weight gain. Evid
Rep. Technol Assess. 2008;168:1–22.
24. Carter JP, Furman T, Hutcheson HR. Preeclampsia and reproductive
performance in a community of vegans. South Med J.
1987;80:692–7.
25. Gabbe SG, Graves CR. Management of diabetes mellitus complicating
pregnancy. Obstet Gynecol. 2003;102:857–68.
26. Jali MV, Desai BR, Gowda S, Kambar S, Jali SM. A hospital
based study of prevalence of gestational diabetes mellitus in an
urban population of India. Eur Rev Med Pharm Sci. 2011;15:
1306–10.
Tomer Avnon 1,2 ● Efrat Paz Dubinsky3 ● Inbar Lavie2 ● Tali Ben-Mayor Bashi1 ● Ronit Anbar3,4 ● Yariv Yogev1,2
Received: 21 April 2020 / Revised: 28 July 2020 / Accepted: 25 August 2020
© The Author(s), under exclusive licence to Springer Nature America, Inc. 2020
Abstract
Objective To determine the effect of a maternal vegan diet on pregnancy outcome.
Study design This is a prospective observational study. Women with a singleton pregnancy who maintained the same diet
prior to, and throughout current pregnancy were enrolled. Stratification was performed according to diet type: vegans,
lacto–ovo–vegetarians, fish-eaters, and omnivores.
Results Overall, 273 women were enrolled, of them, 112 omnivores, 37 fish-eaters, 64 lacto–ovo–vegetarians, and 60
vegans. The vegan diet was significantly associated with an increased risk of small-for-gestational-age newborns compared
only to an omnivore diet (RR = 5.9, 95% CI, 1.2–21.8). The incidence of preterm birth was similar in all groups. Vegans
had lower birthweight compared to lacto–ovo–vegetarians (3015 ± 420 g vs. 3285 ± 482 g, P = 0.004), and to omnivores
(3328 ± 495 g, P < 0.001), but not to fish-eaters. Vegans also had a lower mean gestational weight gain compared only to
omnivores (11.6 ± 4.2 kg vs. 14.3 ± 4.6 kg, P = 0.001).
Conclusion The vegan diet is associated with an increased risk for small-for-gestational-age newborns and lower
birthweight.
Journal of Perinatology
https://doi.org/10.1038/s41372-020-00804-x
ARTICLE
The impact of a vegan diet on pregnancy outcomes
Tomer Avnon 1,2 ● Efrat Paz Dubinsky3 ● Inbar Lavie2 ● Tali Ben-Mayor Bashi1 ● Ronit Anbar3,4 ● Yariv Yogev1,2
Received: 21 April 2020 / Revised: 28 July 2020 / Accepted: 25 August 2020
© The Author(s), under exclusive licence to Springer Nature America, Inc. 2020
Abstract
Objective To determine the effect of a maternal vegan diet on pregnancy outcome.
Study design This is a prospective observational study. Women with a singleton pregnancy who maintained the same diet
prior to, and throughout current pregnancy were enrolled. Stratification was performed according to diet type: vegans,
lacto–ovo–vegetarians, fish-eaters, and omnivores.
Results Overall, 273 women were enrolled, of them, 112 omnivores, 37 fish-eaters, 64 lacto–ovo–vegetarians, and 60
vegans. The vegan diet was significantly associated with an increased risk of small-for-gestational-age newborns compared
only to an omnivore diet (RR = 5.9, 95% CI, 1.2–21.8). The incidence of preterm birth was similar in all groups. Vegans
had lower birthweight compared to lacto–ovo–vegetarians (3015 ± 420 g vs. 3285 ± 482 g, P = 0.004), and to omnivores
(3328 ± 495 g, P < 0.001), but not to fish-eaters. Vegans also had a lower mean gestational weight gain compared only to
omnivores (11.6 ± 4.2 kg vs. 14.3 ± 4.6 kg, P = 0.001).
Conclusion The vegan diet is associated with an increased risk for small-for-gestational-age newborns and lower
birthweight.
Introduction
The number of people who choose to maintain a vegan or
lacto–ovo–vegetarian (LOV) diet and abstain from any
animal-based food has steadily increased over the past few
years. A vegan diet is distinguished from a LOV diet by
being limited to plant-based products and the omission of
dairy products and eggs [1]. Since a vegan diet is different
from LOV diet, it may potentially lead to other nutritional
deficits, depending on supplementation intake, including
vitamins B12 [1–8], B2 [3], and D [4, 5, 7], calcium [5, 7],
iron, zinc [5], and even iodine [6]. The maternal diet during
pregnancy has a direct effect on the newborn’s metabolism,
such as impaired bone mass, during childhood [9], while
low maternal B12 levels associates with insulin resistance,
and changes in lipid profile ratio in the umbilical cord [10].
Few studies have examined the effect of a vegan diet on
pregnancy outcome [11–13]. Although some of them
showed a positive association between birthweight and
maternal consumption of mainly plant-based foods [7, 12],
those studies focused on LOV or on women in the general
population, and not on the vegan population. The data on
the impact of LOV and vegan diets on the gestational age at
delivery, the incidence of preterm delivery [11], as well as
on birthweight [7, 11–15], are inconsistent. The mentioned
studies were performed in different countries with heterogenous
social, cultural, and dietary patterns, which could
influence and cause inconsistent results. In addition, since
vegan women are reportedly at risk of deficiencies of various
vitamin levels, such as B12 and D, their newborns may
also sustain similar deficiencies [8, 11, 12].
In this study, we aimed to determine the association
between specific maternal diet and pregnancy outcome,
especially intrauterine growth restriction and preterm birth,
by comparing women who followed vegan diet to women
who followed lacto–ovo–vegetarian, fish-eaters, and omnivore
diets.
* Tomer Avnon
[email protected]
1 Department of Obstetrics & Gynecology, Lis Maternity &
Women’s Hospital, Tel-Aviv Sourasky Medical Center, affiliated
to the Sackler Faculty of Medicine, Tel-Aviv University,
Tel-Aviv, Israel
2 Sackler Faculty of Medicine, Tel-Aviv University, Tel-Aviv, Israel
3 Nutrition and Dietetic Unit, Tel-Aviv Sourasky Medical Center,
affiliated to the Sackler Faculty of Medicine, Tel-Aviv University,
Tel-Aviv, Israel
4 School of Nutritional Sciences, The Robert H Smith Faculty of
Agriculture, Food and Environmental Quality Sciences, Hebrew
University, Jerusalem, Israel
1234567890();,:
1234567890();,:
Methods
Study population
This prospective observational study of women who gave
birth at a tertiary, university-affiliated medical center was
conducted between May 2018 and June 2019. Eligibility
was limited to women aged 18 years or more with a singleton
pregnancy. Only women who maintained the same
diet for at least 3 months prior to and throughout the current
pregnancy were enrolled. The exclusion criteria were a prior
medical indication for a specific restrictive diet, such as pregestational
diabetes mellitus, celiac disease, lactose intolerance,
and inflammatory bowel disease, and having
undergone bariatric procedures or other bowel resections.
The women were divided into four categories according to
their diet: vegans, who consume only plant-based products,
LOV, who consume mainly plant-based products but also
dairy products and eggs, fish-eaters, who include fish products
in their LOV diet, and omnivores, who consume
animal-based and plant-based products. All the participants
were asked to fill in questionnaires on a diet they followed
throughout their pregnancy. We did not offer any dietary
consultation to prevent interference with the results. The
average caloric and protein intake were for vegans 1984.73 ±
734.91 kcal/day and 59.85 ± 24.15 g/day, for LOV 1773.30 ±
598.90 kcal/day and 60.46 ± 20.71 g/day, for fish-eaters
1809.89 ± 434.03 kcal/day and 68.56 ± 25.19 g/day, and
for omnivores 1733.73 ± 514.45 kcal/day and 78.21 ±
30.95 g/day, respectively. We did not exclude women based
on consumption or not of vitamin supplementation, though
most of the women in all of the diet groups consumed vitamin
supplementation. We recently published that the levels of
vitamin B12 and ferritin levels are similar between pregnant
vegans to LOV and omnivores. Furthermore, we demonstrated
that pregnant vegans who do not consume vitamin
supplementation have lower B12 levels, but still within the
normal range [16].
Data were extracted from the real-time computerized
database and from the filled-in questionnaires. The items
included: eating habits and length of following a specific
diet, maternal age, gravidity, parity, medical information,
vitamins and supplementations taken, body mass index
(BMI) at the time of conception and gestational weight gain
during pregnancy, mode of conception (either spontaneous
or artificial reproductive techniques), mode of delivery, and
gestational age at delivery. Maternal complications included
gestational diabetes mellitus (GDM), defined according to
the American College of Obstetrics and Gynecologists
(ACOG) definitions [17], preeclampsia (PE) and gestational
hypertension, defined according to ACOG definitions [18],
postpartum hemorrhage (PPH), and presence of meconium.
The recorded neonatal information included birthweight and
the 5-min Apgar score. The mean birth percentile for each
neonate was adjusted for gender and gestational age at
delivery according to local population birth curve percentiles
[19]. Primary outcomes were preterm birth (delivery
prior to 37 weeks) and incidence of small-for-gestationalage
(SGA: birthweight below the 10% percentile). Secondary
outcomes were birthweight, the incidence of GDM,
PE, and gestational hypertension, mode of delivery, PPH,
gestational weight gain, and a 5-min Apgar score below 7.
The local institutional review board approved the study
(0715-17-TLV), and all women provided written informed
consent.
Data analysis
Descriptive statistics of demographic and clinical characteristics
were generated by the type of diet followed
during pregnancy. Differences between the selected parameters
of the four study groups were evaluated by one-way
ANOVA and chi-square tests. A hierarchical linear regression
model was used to predict neonatal birthweight and
maternal gestational weight gain among vegans compared
to LOV, fish-eaters, and omnivores, adjusted for maternal
age and BMI. A hierarchical logistic regression model was
used to predict SGA among the neonates of the vegan
mothers compared to the other mothers, adjusted for
maternal age and BMI. Based on the regression model diet
Exp(B) coefficient, we calculated an adjusted relative risk
(RR) for the neonates of vegan mothers to be SGA compared
to the other neonates [20]. A P value of 0.05 was
considered statistically significant. Statistical analysis was
performed with IBM SPSS statistics version 26.
Results
Of the 273 women enrolled in this study, 112 were omnivores,
37 were fish-eaters, 64 were LOV, and 60 were
vegans. The demographic characteristics of the study cohort
are provided in Table 1. The vegan women were older and
had a significantly lower pre-gestational BMI in comparison
to the other groups.
Pregnancy outcomes are provided in Table 2. The
omnivores had the lowest incidence of SGA newborns
(1.79%), and vegans had the highest incidence of SGA
newborns (11.67%, RR = 5.93, 95% CI, 1.20–21.83).
Adjustment for maternal age and pre-pregnancy BMI was
performed due to the demographic differences between
the four groups. The incidence of SGA newborns among the
vegans remained significantly higher compared to the
newborns of the omnivores (95% CI, 0.03–0.71, P =
T. Avnon et al.
0.018), but not compared to the newborns of the LOV (95%
CI, 0.11–1.70, P = 0.236) or fish-eaters (95% CI,
0.25–3.70, P = 0.965). The incidence of preterm birth was
similar in all groups (P = 0.888).
After adjustment for maternal age and pre-pregnancy
BMI, there was a significant difference in neonatal birthweight
between the groups (P = 0.002). The neonatal
birthweight for the vegan group was lower than that for the
LOV group (3015 ± 420 g vs. 3285 ± 482 g, 95% CI,
86.01–440.36, P = 0.004) and that for the omnivore group
(3328 ± 495 g, 95% CI, 142.21–459.34, P < 0.001), but not
for the fish-eaters group (3175 ± 463 g, 95% CI −48.04 to
357.84, P = 0.134); although all mean birthweights were
within the normal range for the local population. After
adjustment for maternal age and pre-pregnancy BMI,
gestational weight gain was significantly different between
the groups (P < 0.001): the vegans had a significantly lower
gestational weight gain in comparison to the omnivores
(11.6 ± 4.2 kg vs. 14.3 ± 4.6 kg, 95% CI, 1.13–4.10, P =
0.001), but not to the fish-eaters (11.2 ± 3.8 kg, 95% CI,
−2.36 to 1.41, P = 0.622), or to the LOV (11.97 ± 4.6 kg,
95% CI, −1.20 to 2.12, P = 0.588).
There was no significant difference between the groups
for the incidence of hypertensive complications of pregnancy
(P = 0.865), GDM (P = 0.546), or cesarean sections
(P = 0.065).
During pregnancy, 30 women received nutritional consultation
(vegans 13.33%, LOV 6.25%, fish-eaters 10.81%,
and omnivores 12.50%). We did not find any influence for
nutritional consultation during pregnancy on any of the
measured outcomes.
Discussion
We aimed to determine the influence on pregnancy outcomes
of the vegan diet in comparison to fish-eaters and
omnivore diets. Our main findings were:
Table 2 Pregnancy outcome according to diet.
Vegan Lacto–ovo–
vegetarian
Fish-eaters Omnivore P value
Characteristic n = 60 n = 64 n = 37 n = 112 (α = 5%)
Gestational weight gain (Kg)# 11.65 ± 4.22 11.97 ± 4.59 11.18 ± 3.84 14.31 ± 4.57 <0.001
GDM, n 8.33% 5 7.81% 5 16.22% 6 8.93% 10 0.546
Week of delivery (weeks) 39.24 ± 1.72 39.49 ± 1.57 39.68 ± 1.33 39.72 ± 1.47 0.237
Number of preterm deliveries (<37 weeks) 5.00% 3 4.69% 3 5.41% 2 3.57% 4 0.888
Delivery by cesarean section, n 20.00% 12 25.00% 16 8.11% 3 12.50% 14 0.065
Hypertensive complications, n 3.33% 2 3.13% 2 2.70% 1 1.79% 2 0.865
Postpartum hemorrhage, n 5.00% 3 9.38% 6 13.51% 5 8.93% 10 0.537
5-min Apgar score ≤7, n 0.00% 0 1.56% 1 0.00% 0 0.00% 0 0.866
Average birthweight (g)# 3015.2 ± 420.4 3285.1 ± 482.3 3175.1 ± 463.4 3328 ± 495.8 0.002
Low birthweight (<2500 g), n 11.67% 0 7.81% 5 8.11% 3 3.57% 4 0.198
Number of SGA (<10%)# 11.67% 7 6.25% 4 10.81% 4 1.79% 2 0.021
Number of SGA (<10%)# P value = 0.236 P value = 0.965 P value = 0.018
Vegan compared to other diet groups.
#Adjusted to age and body mass index (BMI) at pregnancy onset.
GDM gestational diabetes mellitus, SGA small-for-gestational-age.
Table 1 Maternal demographics
according to diet.
Characteristic Vegan Lacto–ovo–vegetarian Fish-eaters Omnivore P value
n= 60 n = 64 n = 37 n = 112 (α = 5%)
Age (years) 34.97 ± 3.85 33.56 ± 4.13 32.62 ± 3.63 32.56 ± 4.02 0.010
BMI 21.41 ± 2.63 23.51 ± 3.42 21.82 ± 2.93 22.56 ± 3.32 0.020
Parity, n (%)
Nullipara 29 48.33% 35 54.69% 24 64.86% 66 58.93% 0.374
Para 1–2 28 46.67% 24 37.50% 11 29.73% 42 37.50% 0.400
Para 3+ 3 5.00% 5 7.81% 2 5.40% 4 3.57% 0.637
Use of ART, n (%) 12 20.0% 11 17.19% 4 10.81% 10 8.93% 0.162
BMI body mass index at pregnancy onset, ART artificial reproductive techniques.
The impact of a vegan diet on pregnancy outcomes
1. Vegans had an increased risk for SGA neonates in
comparison to omnivores and lower mean birthweight
neonates, though within the normal range, in
comparison to omnivores and LOV. In addition,
vegans had lower gestational weight gain in comparison
to omnivores.
2. No difference was found between the four diet groups
for the incidence of hypertensive complications,
GDM, or preterm birth.
Our finding of a lower birthweight among the neonates
of vegans compared to the neonates of omnivores and LOV
are supported by the findings of Ferrara et al. [13] but
apposed conflicting results by others. In the study of Tan
et al. [15], LOV diet did not demonstrate any effect on
birthweight, while Piccoli et al. [11] mentioned heterogenous
birthweights among LOV. Sebastiani et al. [7]
reported a positive relationship between fruit and vegetable
consumption to birthweight, but their study did not specifically
refer to a diet which is completely derived from any
animal-based products. Furthermore, our study is the first to
show a significantly higher incidence of SGA neonates
among vegans, and that the risk remained significant even
after adjustment for maternal age and pre-pregnancy BMI.
Our findings are in agreement with those of Zulyniak et al.
[14], which demonstrated a higher incidence of SGA among
women who consume a plant-based diet, although, like
many other earlier studies, they did not isolate the vegan
population.
Vegans are usually leaner than omnivores [21], and the
vegans in our study also gained less weight during pregnancy
compared to omnivores. This difference might
mediate the lower birthweight among the vegan neonates,
given that women who gain less weight than recommended
are reportedly at risk for having smaller children [22, 23]. It
would follow, therefore, that consulting vegans to aim for
an adequate gestational weight gain might lower that
increased risk for SGA neonates.
We did not find any difference between diet groups in the
duration of pregnancy or in the risk for preterm birth, which
is in agreement with others [11]. We also did not find any
relationship between the vegan diet to hypertensive complications
of pregnancy (either preeclampsia or gestational
hypertension), unlike one previous study that showed a
lower risk among vegans [24]. There is a known association
between increased BMI and prevalence of GDM [25].
While some studies demonstrated a lower risk for GDM
among LOV [7, 26], or mixed results [15], to the best of our
knowledge, no other study has related specifically to the
influence of a vegan diet on the risk for GDM, which we
found to have any effect.
We demonstrated that vegans have an increased risk for
lower neonatal birthweight, albeit within the normal range.
We also found that they had an increased risk for SGA
neonates and for lower gestational weight gain and hypothesized
that the latter might mediate the birthweight differences.
Therefore, we think that our findings should not be
used to persuade vegans to abandon their diets, but rather
that they be encouraged to maintain a healthy diet and to
undergo regular follow-up of maternal weight and fetal
weight estimation and to undergo specific diet consultation.
The strengths of our study are that it is one of the largest
on pregnancy outcomes that focused specifically on the
vegan population. Unlike many past studies that combined
vegans and LOV, or that had only a few vegan patients, our
study differentiated them from LOV in the evaluations of all
the selected parameters. We prevented contamination of the
results by restricting the study to women who followed the
same diet for at least 3 months prior to their pregnancy up to
delivery. We also recruited women during different stages
of their pregnancy in order to maintain heterogenicity and to
prevent selection bias.
Our study has some limitations that bear mention.
Although it is one of the largest studies of its kind, we were
not able to stratify other demographic characteristics, such
as education, alcohol consumption, and smoking. We also
excluded women who began their pregnancy while following
a vegan or LOV diet and changed it during the
course of pregnancy. Thus, precluding our ability to determine
whether there is a specific point in pregnancy in which
a change in diet might influence the outcomes.
Our findings suggest that a vegan diet is associated with
an increased risk for SGA and lower-birthweight neonates
and with lower gestational weight gain. Vegan women
should be encouraged to maintain a healthy diet, consult a
dietician, followed regularly for fetal growth, including
sonographic screening for intrauterine growth restriction
and followed for adequate gestational weight gain during
their pregnancy.
Funding No funding was received.
Author contributions Tomer Avnon—conception, methodology,
investigation supervision, data curation, formal analysis, and drafting
the initial paper. Efrat Paz Dubinsky—investigation and data curation.
Inbar Lavie—formal analysis. Tali Ben-Mayor Bashi—investigation
and data curation. Ronit Anbar—methodology and investigation.
Yariv Yogev—methodology, investigation supervision, and resources.
All authors revised the paper, gave final approval of the version to be
published, and agreed to be accountable for all aspects of the work.
Compliance with ethical standards
Conflict of interest The authors declare that they have no conflict of
interest.
Publisher’s note Springer Nature remains neutral with regard to
jurisdictional claims in published maps and institutional affiliations.
T. Avnon et al.
References
1. Key TJ, Appleby PN, Rosell MS. Health effects of vegetarian and
vegan diets. Proc Nutr Soc. 2006;65:35–41.
2. Gilsing AMJ, Crowe FL, Lloyd-Wright Z, Sanders TAB, Appleby
PN, Allen NE, et al. Serum concentrations of vitamin B12 and
folate in British male omnivores, vegetarians and vegans: results
from a cross-sectional analysis of the EPIC-Oxford cohort study.
Eur J Clin Nutr. 2010;64:933–9.
3. Majchrzak D, Singer I, Männer M, Rust P, Genser D, Wagner KH,
et al. B-vitamin status and concentrations of homocysteine in
Austrian omnivores, vegetarians and vegans. Ann Nutr Metab.
2007;50:485–91.
4. Elorinne AL, Alfthan G, Erlund I, Kivimäki H, Paju A, Salminen
I, et al. Food and nutrient intake and nutritional status of Finnish
vegans and non-vegetarians. PLoS ONE. 2016;11:1–14.
5. Winston CJ. Health effeets of vegan diets 1-3. Am J Clin Nutr.
2009;89:1627–33.
6. Leung AM, LaMar A, He X, Braverman LE, Pearce EN. Iodine
status and thyroid function of Boston-area vegetarians and vegans.
J Clin Endocrinol Metab. 2011;96:1303–7.
7. Sebastiani G, Barbero AH, Borrás-Novel C, Casanova MA,
Aldecoa-Bilbao V, Andreu-Fernández V, et al. The effects of
vegetarian and vegan diet during pregnancy on the health of
mothers and offspring. Nutrients. 2019;11:1–29.
8. Pawlak R. To vegan or not to vegan when pregnant, lactating or
feeding young children. Eur J Clin Nutr. 2017;71:1259–62.
9. Ganpule A, Yajnik CS, Fall CHD, Rao S, Fisher DJ, Kanade A,
et al. Bone mass in Indian children—relationships to maternal
nutritional status and diet during pregnancy: the Pune maternal
nutrition study. J Clin Endocrinol Metab. 2006;91:2994–3001.
10. Adaikalakoteswari A, Vatish M, Lawson A, Wood C, Sivakumar
K, McTernan PG, et al. Low maternal vitamin B12 status is
associated with lower cord blood HDL cholesterol in white caucasians
living in the UK. Nutrients. 2015;7:2401–14.
11. Piccoli GB, Clari R, Vigotti FN, Leone F, Attini R, Cabiddu G,
et al. Vegan-vegetarian diets in pregnancy: danger or panacea? A
systematic narrative review. BJOG Int J Obstet Gynaecol.
2015;122:623–33.
12. Pistollato F, Sumalla Cano S, Elio I, Masias Vergara M, Giampieri
F, Battino M. Plant-based and plant-rich diet patterns during
gestation: beneficial effects and possible shortcomings. Adv Nutr.
2015;6:581–91.
13. Ferrara P, Sandullo F, Di Ruscio F, Franceschini G, Peronti B,
Blasi V, et al. The impact of lacto-ovo-/lacto-vegetarian and vegan
diets during pregnancy on the birth anthropometric parameters of
the newborn. J Matern Neonatal Med. 2019;0:1–7.
14. Zulyniak MA, De Souza RJ, Shaikh M, Desai D, Lefebvre DL,
Gupta M, et al. Does the impact of a plant-based diet during
pregnancy on birth weight differ by ethnicity? A dietary pattern
analysis from a prospective Canadian birth cohort alliance. BMJ
Open. 2017;7:1–9.
15. Tan C, Zhao Y, Wang S. Is a vegetarian diet safe to follow during
pregnancy? A systematic review and meta-analysis of observational
studies. Crit Rev Food Sci Nutr. 2019;59:2586–96.
16. Avnon T, Anbar R, Lavie I, Ben-Mayor Bashi T, Paz Dubinsky E,
Shaham S, et al. Does vegan diet influence umbilical cord vitamin
B12, folate, and ferritin levels? Arch Gynecol Obstet.
2020;301:1417–22.
17. Committee on Practice Bulletins—Obstetrics. ACOG Practice
Bulletin No. 190: Gestational diabetes mellitus. Obstet Gynecol.
2018;131;e49–64.
18. Committee on Practice Bulletins—Obstetrics. ACOG Practice
Bulletin No. 202: Gestational hypertension and preeclampsia.
Obstet Gynecol. 2019;133:e1–25.
19. Dollberg S, Haklai Z, Mimouni FB, Gorfein I, Gordon E-S. Birth
weight standards in the live-born population in Israel. Isr Med
Assoc J. 2005;7:311–4.
20. Zhang J, Yu KF. What’s the relative risk? A method of correcting
the odds ratio in cohort studies of common outcomes. J Am Med
Assoc. 1998;280:1690.
21. Rosell M, Appleby P, Spencer E, Key T. Weight gain over 5 years
in 21 966 meat-eating, fish-eating, vegetarian, and vegan men and
women in EPIC-Oxford. Int J Obes. 2006;30:1389–96.
22. Goldstein RF, Abell SK, Ranasinha S, Misso M, Boyle JA, Black
MH, et al. Association of gestational weight gain with maternal
and infant outcomes: a systematic review and meta-analysis. J Am
Med Assoc. 2017;317:2207–25.
23. Viswanathan M, Siega-Riz AM, Moos MK, Deierlein A, Mumford
S, Knaack J, et al. Outcomes of maternal weight gain. Evid
Rep. Technol Assess. 2008;168:1–22.
24. Carter JP, Furman T, Hutcheson HR. Preeclampsia and reproductive
performance in a community of vegans. South Med J.
1987;80:692–7.
25. Gabbe SG, Graves CR. Management of diabetes mellitus complicating
pregnancy. Obstet Gynecol. 2003;102:857–68.
26. Jali MV, Desai BR, Gowda S, Kambar S, Jali SM. A hospital
based study of prevalence of gestational diabetes mellitus in an
urban population of India. Eur Rev Med Pharm Sci. 2011;15:
1306–10.