Dessert_All_Day
Member
- Joined
- May 26, 2016
- Messages
- 406
Follow along with the video below to see how to install our site as a web app on your home screen.
Note: This feature may not be available in some browsers.
Click Here if you want to upgrade your account
If you were able to post but cannot do so now, send an email to admin at raypeatforum dot com and include your username and we will fix that right up for you.
So should I throw my coconut oil away ?
Doesn't matter. What is more associated with cardiovascular disease is Lp(a). They use HDL as a proxy because because it ignores the vitamin C connection:
A Unified Theory of Human Cardiovascular
Disease Leading the Way to the Abolition of
This Disease as a Cause for Human Mortality
Matthias Rath M.D. and Linus Pauling Ph.D.
Solution of the puzzle of human cardiovascular disease: Its primary
cause is ascorbate deficiency, leading to the deposition of
lipoprotein(a) and fibrinogen/fibrin in the vascular wall.
Matthias Rath M.D. and Linus Pauling Ph.D.
I would listen to Linus Pauling over Stephen Nutella anyday, and especially in this case as the Pauling/Rath theory actually makes sense.
Mice don't. From the article Animal Models of Cardiovascular Diseases:If vitamin C deficiency is the main cause of CVD then why do animals who can synthesize their own get it too?
PUFA, and hypothyroidism, seem like a much more likely cause. Which would explain the rise in CVD in pets who eat conventional pet food.
ugs [4]. As wild-type mice are resistant to lesion development, the current mouse models for atherosclerosis are based on genetic modifications of lipoprotein metabolism with additional dietary changes.
2.1.3. Dogs: The dog can appear to be an attractive species for the study of CVD and has, in the past, been widely used for studies of circulatory physiology. However, while dogs can be of an ideal size and are easy to work with, there are problems associated with the status of dogs in the Western culture and with anthropomorphic attitudes toward them [29]. In addition, as canines, they are carnivores and are, in turn, resistant to high-lipid diets and atherosclerosis.
The normal rat, like the dog, is typically resistant to the development of atherosclerosis, and this has led to the notion that the rat is not a suitable subject for cardiovascular research.
I didn't think that gelatin had any lysine. All you need is vitamin C. It is uncrosslinked scruffy degraded collagen on the arterial walls that binds with Lp(a) and initiates plaque formation. Vitamin C upregualtes procollagen synthesis threefold and is necessary for crosslinking collagen in the arterial wall and elsewhere.
If you were to believe the mainstream theory, the one that the sell the public, then you would have to explain why athersclerosis occurs in the arteries. These are the high-pressure areas. The veins are the low-pressure areas.
If HDL clogged the vasculature merely by its presence, you would expect it to clog the low-pressure areas first. This is not what is seen. What happens is that the high-pressure areas that suffer the most damage are attacked first.
George Willis discovered this long before Pauling did in guinea pigs. When you hold vitamin C away from guinea pigs they eventually die via internal hemorrhage.
• AN EXPERIMENTAL STUDY OF THE INTIMAL GROUND SUBSTANCE IN ATHEROSCLEROSIS
• SERIAL ARTERIOGRAPHY IN ATHEROSCLEROSIS
• ASCORBIC ACID CONTENT OF HUMAN ARTERIAL TISSUE
• THE REVERSIBILITY OF ATHEROSCLEROSIS
Vitamin C keeps the arteries' collagen strong and crosslinked. It stays smooth and no amount of LDL can stick to it.
Isn't the Lp(a) there mopping up the oxidized LDL particles? And it's the PUFA in the phospholipids of the LDL membrane that get oxidized. So like @tca300 suggested, low PUFA diet plus good metabolic rate to metabolize LDL particles quickly should reduce the chances of LDL oxidation.It is uncrosslinked scruffy degraded collagen on the arterial walls that binds with Lp(a) and initiates plaque formation.
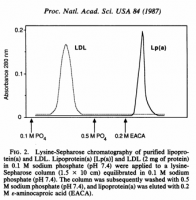
Polymorphic forms of Lp(a) with different structural and functional properties: cold-induced self-association and binding to fibrin and lysine-SepharoseAutologous LDL, Lp(a) and d-Lp(a) were isolated from the plasma of a subject with two isoforms of apo(a). Briefly, the lipoproteins contained in 1 1 of plasma were floated at d = 1.21 g/ml and applied to a lysine-Sepharose column (20 × 5 cm2), which was equilibrated with 33 mM phosphate, 1 mM benzamidine, 0.01% Na2-EDTA, 0.01% NAN3, pH 7.4.
The word scurvy probably originated from the Middle Low German word schorbuk which came from schoren, “break”, and buk, “belly” referring to the phenomenon observed among the seafarers during the long sea voyages of the 15th to 18th centuries, where old healed scars and wounds would disintegrate, some leading to a “ruptured belly”.
The prominent feature of scurvy is tissue bleeding with nonpalpable purpura. Hodges et al studied the onset and progression of scurvy in humans in a study of 5 male volunteers from the Iowa State Penitentiary whose diets were strictly controlled. Symptoms appeared 29 to 90 days after deprivation of vitamin C. The first sign to appear was petechial hemorrhage.
And Nutella has too much PUFAs anyway. Here you go: Lily's Coconut Jam 275gI would listen to Linus Pauling over Stephen Nutella anyday, and especially in this case as the Pauling/Rath theory actually makes sense.
Obesity (four of the five dogs), diabetes mellitus (one dog), male gender (all five dogs) and advanced age (four dogs) were considered to be risk factors for atherosclerosis in the present study. Because the number of aged and obese dogs is likely to increase in the future, it seems possible that atherosclerosis may become an important disease of dogs.
Atherosclerosis is the most common vascular disease of man, with important complications such as ischaemic heart disease, myocardial and cerebral infarction, stroke, and gangrene of extremities. It is less significant in domestic animals, with the exception of rabbits, chickens, and pigs. Systemic atherosclerosis is uncommon in animals, and almost always occurs in association with hypothyroidism.
Almost 100 years ago, some experiments in Russia showed that feeding rabbits cholesterol caused them to develop atherosclerosis, but subsequent experiments showed that rabbits are unusual in responding that way to cholesterol, and that even rabbits don't develop atherosclerosis from cholesterol if they are given a supplement of thyroid (Friedland, 1933). By 1936, it was clear that hypercholesterolemia in humans and other animals was caused by hypothyroidism, and that hypothyroidism caused many diseases to develop, including cardiovascular disease and cancer. There was already more reason at that time to think that the increased cholesterol was a protective adaptation than to think that it was maladaptive.
The strange idea that cholesterol causes atherosclerosis was revived in the 1950s when the vegetable oil industry learned that their polyunsaturated oils lowered serum cholesterol. (Many other toxins lower cholesterol, but that is never mentioned.) The industry began advertising their oils as "heart protective," and they enlisted some influential organizations to help in their advertising: The American Dietetic Association, the American Heart Association, the US Dept. of Agriculture and FDA, and the AMA. Besides the early rabbit research, which didn't make their case against cholesterol and might actually have had implications harmful to their argument (since Anitschkow had used vegetable oil as solvent for his cholesterol feedings), the oil industry helped to create and promote a large amount of fraudulent and unscientific work.
Guy that has written the article has founded a society for "skeptical people" yet he follows the mainstream beliefs of saturated fat without a hint of skepticism.